It was the 3rd January 2016, we had just finished the Christmas festivities, always a big thing in our house, my wife Joanne (Jo) is Christmas mad. We always have a house full of  family and friends.
family and friends.
There was no previous history of breast cancer in Jo’s family, so I don’t believe she checked her breasts religiously but as she was adjusting the strap on her nightdress she felt a lump that she hadn’t felt before. I remember Jo being immediately filled with dread, she somehow knew straight away it wasn’t good.
The next morning we were up early (I don’t think we slept much) and managed to book an emergency appointment with our GP for later that day. We saw our GP and he said he thought it was probably a cyst or something harmless but would refer us to the breast clinic to be checked. That put our minds a little at rest, which made the two week wait for the Breast clinic a little easier.
The appointment at the breast clinic didn’t go well, they confirmed something was suspicious but until the biopsy came back they wouldn’t know if it was benign or not. What followed was the longest two weeks of our lives as we waited for the biopsy result, going from being convinced it was cancer, to thinking it would all be ok and back again.
We went to the results appointment in Brighton and were ushered in to a room by a nurse who turned out to be a macmillan nurse and an oncologist, to be told the dreaded words that the lump was indeed cancer and a fairly aggressive one, Stage 3 Triple negative Breast cancer.
At that point your life is turned upside down. I found myself reverting to how I might handle a problem at work, look for solutions, try and get some information so I could inform myself and understand what to expect but really I think my mind was all a bit of a blur during that initial meeting. Jo’s initial gut feeling had been correct, while I had spent much of that previous 4 weeks in a state of denial.
Jo surprised me by being very positive at that point, (I am the glass half full guy and she is more glass half empty) the oncologist said that they were aiming for a cure and she hung on to that and then started to focus quickly on what appointments were next and look forward.
A number of scans followed and when the results came back it confirmed it was local to the breast but there was something in the bladder that should be checked but they said it wouldn’t be related.
What followed was 6 sessions of FEC-T chemotherapy, a lumpectomy with lymph node removal and then 20 sessions of radiotherapy. She lost all her curly hair, but coped pretty well with all the side effects and the strain of constant appointments.
During this period the ‘thing’ in the bladder also turned out to be cancer, though another primary, although this one was slow growing and not too much to worry about, she had the cancer polyps removed in an operation but was able to go home the same day.
Jo was the model patient, every time she went to the oncologist he would say how she was the ideal patient as she coped with everything so well and once the cancer was gone she continued to get back to normal life and fitness without much delay.
After all the treatment she took up swimming to help her recover and would think nothing of going to the pool and doing 100 or even 200 lengths. She did Race for life’s Pretty Muddy with our daughter and we did the shine walk to give a bit back to Cancer Research.
.


So everything was going pretty well as we went through 2017, cancer free, back at work, enjoying life. We started a habit of going away every month for at least 1 night which helped bring us even closer together. You will hear more about these nights away throughout my twitter feed and this blog.
The only real issue she had following the 2016 treatments had been a number of Seroma’s following the lumpectomy and some internal scarring following radiotherapy which had left her breast hard in places. This hardness meant we couldn’t be sure always of whether something was suspicious or not but the 2017 follow up mammogram had given us the all clear.
So we came in to 2018 and things started to go wrong again. Firstly her right nipple started to have occasional discharge of seroma like fluid and also we felt that the scarring ‘lump’ from radiotherapy was not quite the same as before. So we went back to the oncologist who assured us it looked fine but arranged a mammogram and an ultrasound just to be sure. In March the results were confirmed as being all ok to our relief.
In April we were on a family trip to Ireland when the nipple started to show further signs of problems and small lumps started to appear. On return Jo didn’t want to immediately go back to the oncologist as she had only been to see him weeks before and didn’t want to make a fuss so she booked an appointment with the GP surgery. As I expected the GP’s immediately referred us back to the oncologist. However we had seen him less than 2 months ago so surely it couldn’t be the cancer!
However as the appointment got closer, I started to feel more worried as the lumps to me looked sore and angry and I couldn’t think of too many other things it could be. Google didn’t help allay the fears.
So we went in and saw the oncologist and his first words on examining her were ‘you were right to come in, you were right to be worried, I am worried, I think this is the cancer returning’.
So there started a few days of scans and biopsies, all quickly done due to the power of private health cover and then back for confirmation that the cancer had not only returned to the original right breast but was also now in the other breast and lymph nodes on the left side and neck.
In the same results consultation we were told that the treatment to follow would be a double mastectomy, lymph node clearance, chemotherapy and radiotherapy. In fact the hospital had a cancellation and she could go in for the double mastectomy in 48 hours. It was all a huge amount to take in. The oncologist, breast nurse and hospital matron advised us that it was completely up to us, they appreciated it was a rush but to have a think about it and come back the next day. If we didn’t want to do it then it would only be a week or so anyway so the decision was up to us.
We walked out of there again a bit shell shocked. Things had happened so quickly in the space of a couple of weeks, we had gone from being fine to facing a large operation and a cancer that was misbehaving, spreading quickly and generally being a pain the backside.
The decision on the operation we made in the 40 minute drive home, what was the point of waiting, the sooner it happened the sooner she would be cancer free.
We rang the next morning to confirm we would be there.
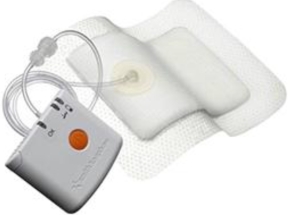
The operation went well, no drains were required, just these very clever bandages, (Pico dressing) she was home the next day within 24 hours of entering the hospital. As I said before she is the ‘model patient!’
The only disappointment was that they didn’t quite get all of it, there is a small lump left in her neck, which they intend to target with the chemo and radiotherapy.
All went well with recovery apart from some Seroma’s which needed draining on a few occasions by the surgeon. She keeps a tally on how much each time, 700ml was the biggest.
After about a month recovery, chemo started, Carboplatin intravenously once every 3 weeks for 6 cycles and for each of those cycles there would be 2 weeks worth of capecitabine orally.
Cycle 1 she strolled through apart some slight pain to her hands and feet a well known side effect of the Capecitabine.
Cycle 2 started fine, but during week 2 Jo developed this strange rash starting around the left sided mastectomy scar and quickly spread across and up her chest and round her left side.
Initially it was thought to be an infection but it didn’t seem to respond to antibiotics and had steadily got worse by the time we were back at the unit for pre-chemo bloods.
The nurses and matron had a look at it and decided it was best if we returned that evening to see the oncologist.
I had done some research and decided in my wisdom that it was a form of purpura caused by low platelet count so went to the consultation not particularly worried but hoping it wouldn’t delay the chemo too much.
We got there to be greeted by both the breast care nurse, the matron who is also a breast care nurse and the oncologist. He examined Jo and then dropped the bombshell that the rash in his opinion had the hallmarks of inflammatory breast cancer, that was rapidly spreading. The chemo would stop, they would do tests to confirm, but the nurses had felt the same which was why they had alerted him.
The reality was that the chemo wasn’t working, the cancer was rapidly spreading and that a trial would be our only hope, if one was available.
The oncologist and nurses were very kind and supportive, they wished it wasn’t the case but we had a plan, it was Monday night about 9:15, we would be back tomorrow for a biopsy to confirm and a CT scan to see where else it had gone. Thursday Jo would have a blood transfusion as her red blood count was very low and we would see the oncologist again to find out the results and see if any trial was available.
The oncologist asked if I had any questions, I replied that there were none that I suspected I wanted to know the answer too at this stage.
So we left the hospital in tears for the drive home. Deciding what we should tell the kids, what could we do? Wondering if it was the start of the end.
Many tears were shed that night, we told the kids, we have always been open and honest they are 19 and 14 so could understand and anyway they are not stupid they would wonder why we were crying. We let other members of our immediate family know that things had taken a turn for the worse. We began to prepare ourselves for what lay ahead.
The next day we had a late appointment with the surgeon for the biopsy and had the CT scan just before it. Accompanying the surgeon was our breast care nurse, who had seen us the previous day. We had thought ourselves earlier that the rash hadn’t looked quite so bad but thought that maybe was just a trick of the light but when she saw it, she also agreed that it looked lighter than the previous day. When the surgeon came in he immediately said he didn’t think it looked as bad as he expected and was possibly still an infection. A glimmer of hope was back in our lives.

The Thursday saw us arrive at the hospital reasonably early for the blood transfusion and the nurse again came in to see us, by now the rash had reduced significantly and she like us was more positive. The oncologist then came to the ward to see us with the news that the CT scan was clear and that if it was inflammatory breast cancer he would expect to see it worsening rapidly and not improving. If as expected the biopsy was clear we would be back on track the following week with the planned chemo.
He apologised for getting it wrong and putting us through the previous few days but he was delighted he turned out to be wrong. We are still not 100% sure what it was, possibly a reaction of the infection to the low platelets but the relief we felt that day was truly amazing.
Cycle 3 went without a hitch, the blood transfusion she had that previous week had given Jo a great physical lift and she sailed through the cycle.
Cycle 4, well this is where we are now. Jo is a bit tired and her feet are playing up a bit but apart from that she is good and still looks amazing.
Next appointment is the oncologist again on 30th August, fingers crossed!!
Please follow my twitter feed for regular updates http://www.twitter.com/cancerhusband1

A true and heart rendering account. No- one knows the fear and dread till they have sat in that chair hanging on the consultants every word. At the same time just managing to breath !!! It is as hard for those surrounding the patient and emotionally draining. Well done for doing this upfront and deep insight into Jo’s journey with cancer.
LikeLike
Thanks Fiona for your comment. The feedback is much appreciated.
LikeLike
OMG you two are amazing to hear all that you have been through and are still going through is really hard. You never want to think of any of your friends going through something like this. You are such a gorgeous loved up pair and we miss seeing you at the local. Big hugs and all the best you are both awesome 😍😘xx
LikeLike
Thanks Emma. Miss you guys too. X
LikeLike
[…] How we got here – Our story so far […]
LikeLike